Acute Liver Failure | Vibepedia
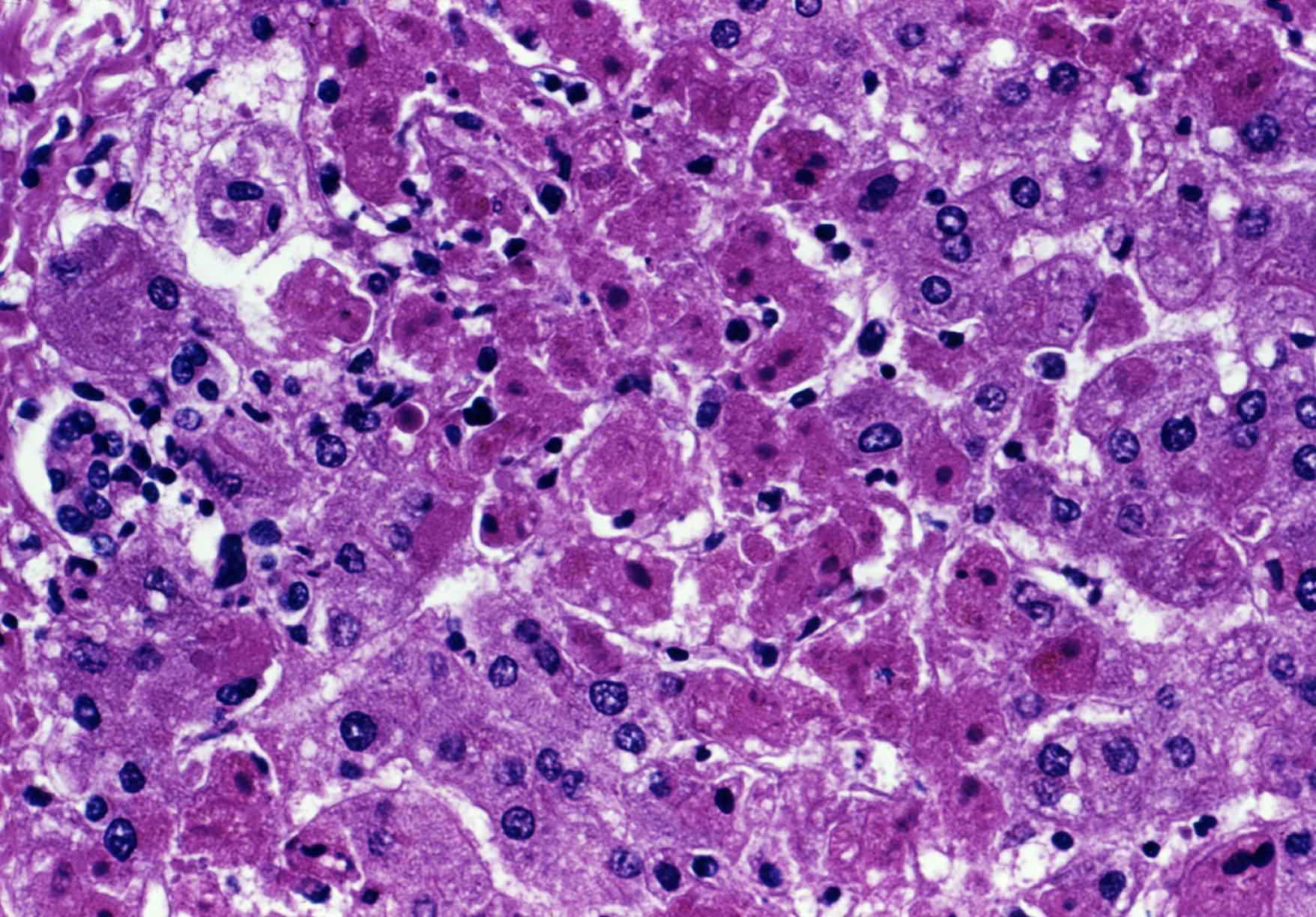
Acute liver failure (ALF) is a rare but catastrophic medical emergency characterized by the rapid deterioration of liver function, typically within days or…
Contents
- 🎵 Origins & History
- ⚙️ How It Works
- 📊 Key Facts & Numbers
- 👥 Key People & Organizations
- 🌍 Cultural Impact & Influence
- ⚡ Current State & Latest Developments
- 🤔 Controversies & Debates
- 🔮 Future Outlook & Predictions
- 💡 Practical Applications
- 📚 Related Topics & Deeper Reading
- Frequently Asked Questions
- References
- Related Topics
Overview
The concept of rapid, severe liver damage has been recognized for centuries, though the formal definition of acute liver failure is a more recent development. Early descriptions often conflated ALF with fulminant hepatic failure, particularly in the context of infectious diseases like yellow fever, which caused widespread liver necrosis. The 20th century saw a growing understanding of toxic insults, especially from industrial chemicals and later, pharmaceuticals. The identification of [[acetaminophen-overdose|acetaminophen]] as a potent hepatotoxin in the 1960s and 70s, particularly after the work of [[vincent-connolly|Vincent Connolly]] and others, revolutionized the understanding of drug-induced ALF. The seminal classification by [[laith-al-mossy|Laith Al-Mossy]] and colleagues in 1993 provided a standardized framework, distinguishing between hyperacute, acute, and subacute presentations based on the time to [[jaundice|jaundice]] development, which significantly impacted prognosis and management strategies at institutions like [[king's-college-hospital|King's College Hospital]] in London.
⚙️ How It Works
At its core, acute liver failure is a massive, rapid loss of functional [[hepatocytes|liver cells]]. This cellular destruction triggers a cascade of systemic failures. The liver's inability to detoxify ammonia and other neurotoxins leads to [[hepatic-encephalopathy|hepatic encephalopathy]], manifesting as confusion, altered consciousness, and potentially [[coma|coma]]. Impaired synthesis of vital proteins, such as albumin and clotting factors, results in [[hypoalbuminemia|hypoalbuminemia]] (low blood albumin) and [[coagulopathy|coagulopathy]] (impaired blood clotting), increasing the risk of bleeding and edema. The liver's role in glucose homeostasis is compromised, leading to [[hypoglycemia|hypoglycemia]]. Furthermore, the inflammatory response to massive hepatocellular injury can trigger [[systemic-inflammatory-response-syndrome|SIRS]] and multi-organ dysfunction, affecting the kidneys, lungs, and cardiovascular system. The speed of this collapse is what defines ALF, distinguishing it from chronic liver diseases like [[cirrhosis|cirrhosis]].
📊 Key Facts & Numbers
Acute liver failure affects approximately 5-10 individuals per million population annually worldwide. In the United States and Europe, [[acetaminophen-overdose|acetaminophen]] overdose accounts for over 50% of ALF cases, with an estimated 80,000 cases of acetaminophen-induced liver injury reported annually in the US alone. Viral hepatitis, particularly [[hepatitis-a|Hepatitis A]], [[hepatitis-b|Hepatitis B]], and [[hepatitis-e|Hepatitis E]], contributes significantly to global ALF incidence, especially in developing nations where vaccination rates are lower. Autoimmune hepatitis is responsible for about 10-15% of cases in Western countries. The mortality rate for ALF without [[liver-transplantation|liver transplantation]] can exceed 70%, but this figure drops to around 30-40% with successful transplantation. Survival rates for hyperacute ALF due to [[acetaminophen-overdose|acetaminophen]] can reach up to 80% with prompt [[n-acetylcysteine|N-acetylcysteine]] treatment.
👥 Key People & Organizations
Key figures in understanding and managing ALF include [[laith-al-mossy|Laith Al-Mossy]], whose 1993 classification remains influential, and [[vincent-connolly|Vincent Connolly]], a pioneer in recognizing acetaminophen's hepatotoxicity. Organizations like the [[american-association-for-the-study-of-liver-diseases|American Association for the Study of Liver Diseases (AASLD)]] and the [[european-association-for-the-study-of-the-liver|European Association for the Study of the Liver (EASL)]] are crucial in developing clinical guidelines and promoting research. Major transplant centers, such as [[university-of-pittsburgh-medical-center|UPMC]] in Pittsburgh and [[stanford-university-medical-center|Stanford Hospital]], are at the forefront of liver transplantation and ALF management. The [[national-institute-of-diabetes-and-digestive-and-kidney-diseases|National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK)]] funds significant research into liver diseases, including ALF.
🌍 Cultural Impact & Influence
Acute liver failure, while medically defined, has seeped into popular culture primarily through dramatic medical dramas and news reports highlighting its sudden and devastating nature. Films like 'Awake' (2007) have depicted characters experiencing severe medical complications, sometimes touching on organ failure, though often with dramatic license. The stark reality of ALF serves as a potent reminder of the liver's vital, yet often overlooked, role in maintaining life. Public health campaigns focused on safe [[acetaminophen-use|acetaminophen]] consumption and [[hepatitis-vaccination|hepatitis vaccination]] indirectly raise awareness about the conditions that can lead to ALF. The urgency of ALF also underscores the critical importance of organ donation and the [[united-network-for-organ-sharing|United Network for Organ Sharing (UNOS)]] in facilitating life-saving [[liver-transplantation|liver transplants]].
⚡ Current State & Latest Developments
Current research is intensely focused on improving prognostication and developing novel therapeutic strategies beyond transplantation. Biomarkers that can predict the likelihood of spontaneous recovery versus the need for transplant are a major area of investigation, aiming to refine decision-making for [[liver-transplantation|liver transplantation]]. Efforts are underway to develop [[bioartificial-liver-devices|bioartificial liver devices]] that can support liver function temporarily, bridging patients to recovery or transplant. Furthermore, understanding the intricate immune responses in ALF is crucial for developing immunomodulatory therapies. The [[hepatitis-c-virus|Hepatitis C]] crisis has seen a rise in ALF cases related to [[drug-induced-liver-injury|drug-induced liver injury]] from illicit substances, prompting closer monitoring by public health bodies like the [[centers-for-disease-control-and-prevention|CDC]].
🤔 Controversies & Debates
A significant debate revolves around the optimal timing and criteria for [[liver-transplantation|liver transplantation]] in ALF patients, particularly those with indeterminate prognoses. The scarcity of donor organs means difficult ethical decisions must be made daily. Another controversy lies in the management of [[acetaminophen-overdose|acetaminophen]] poisoning; while [[n-acetylcysteine|N-acetylcysteine]] is highly effective, its optimal dosing and duration, especially in chronic overdose scenarios, are still refined. The role of alternative therapies, such as [[stem-cell-therapy|stem cell therapy]] for liver regeneration, remains a subject of intense research and debate, with many early-stage trials showing promise but lacking definitive clinical proof for ALF.
🔮 Future Outlook & Predictions
The future of ALF management hinges on personalized medicine and advanced technological solutions. Predictive algorithms incorporating genetic predispositions, detailed clinical data, and novel biomarkers will likely improve prognostication accuracy. The development and widespread adoption of more sophisticated [[bioartificial-liver-devices|bioartificial liver devices]] could significantly reduce the reliance on scarce donor organs. Furthermore, advancements in [[gene-therapy|gene therapy]] and [[regenerative-medicine|regenerative medicine]] may offer future possibilities for repairing damaged liver tissue, potentially obviating the need for transplantation in select cases. Research into the gut-brain axis in ALF may also unlock new therapeutic targets for managing [[hepatic-encephalopathy|hepatic encephalopathy]].
💡 Practical Applications
The primary practical application of understanding ALF is in its immediate medical management. This includes rapid diagnosis through blood tests measuring [[liver-enzymes|liver enzymes]], [[prothrombin-time|prothrombin time]], and [[serum-albumin|serum albumin]] levels, alongside clinical assessment for [[hepatic-encephalopathy|hepatic encephalopathy]]. Prompt administration of antidotes, such as [[n-acetylcysteine|N-acetylcysteine]] for acetaminophen overdose, is critical. Intensive care unit (ICU) support is essential for managing complications like cerebral edema, coagulopathy, and infections. For patients not recovering spontaneously, the crucial application is the timely referral for [[liver-transplantation|liver transplantation]], a complex surgical procedure requiring meticulous donor matching and post-operative care coordinated by teams at specialized [[transplant-centers|transplant centers]].
Key Facts
- Year
- 20th Century (formal definition)
- Origin
- Global
- Category
- science
- Type
- topic
Frequently Asked Questions
What are the main causes of acute liver failure?
The primary causes of acute liver failure vary geographically. In Western countries, [[acetaminophen-overdose|acetaminophen]] poisoning is the leading cause, accounting for over 50% of cases. Globally, [[viral-hepatitis|viral hepatitis]] (especially [[hepatitis-b|Hepatitis B]] and [[hepatitis-e|Hepatitis E]]) is a major contributor, particularly in regions with lower vaccination rates. [[Autoimmune-hepatitis|Autoimmune hepatitis]], idiosyncratic drug reactions, and toxins like [[amanita-phalloides|Amanita phalloides]] mushrooms are also significant causes. The specific etiology dictates the urgency of treatment and the potential for spontaneous recovery.
How is acute liver failure diagnosed?
Diagnosis of acute liver failure relies on a combination of clinical presentation and laboratory findings. Key indicators include the rapid onset of [[jaundice|jaundice]] within weeks of initial liver injury, coupled with severe [[coagulopathy|coagulopathy]] (indicated by a [[prothrombin-time|prothrombin time]] of >5 seconds above control or an [[international-normalized-ratio|INR]] >1.5) and [[hepatic-encephalopathy|hepatic encephalopathy]] (altered mental status). Blood tests will also show elevated [[liver-enzymes|liver enzymes]] like [[alanine-aminotransferase|ALT]] and [[aspartate-aminotransferase|AST]], though these may normalize or even decrease in the late stages due to a depleted liver cell reserve. [[Serum-albumin|Serum albumin]] levels will be low due to impaired synthesis.
What are the survival rates for acute liver failure?
Survival rates for acute liver failure are highly variable and depend heavily on the underlying cause, the speed of treatment, and whether a [[liver-transplantation|liver transplant]] is performed. Without transplantation, mortality can exceed 70%. However, with prompt treatment, particularly [[n-acetylcysteine|N-acetylcysteine]] for [[acetaminophen-overdose|acetaminophen]] poisoning, survival rates can reach up to 80%. For patients requiring a transplant, survival rates post-transplantation are generally around 60-70%, though this can vary based on the patient's overall condition and the availability of suitable donor organs. Early referral to a specialized [[transplant-center|transplant center]] is crucial for improving outcomes.
Can the liver recover from acute liver failure?
Yes, spontaneous recovery from acute liver failure is possible, especially in cases caused by [[acetaminophen-overdose|acetaminophen]] poisoning treated promptly with [[n-acetylcysteine|N-acetylcysteine]], or in certain forms of viral hepatitis. The liver possesses a remarkable capacity for regeneration. However, the likelihood of recovery is strongly influenced by the extent of initial damage and the speed of intervention. If 80-90% of liver cells are destroyed, the remaining healthy cells must proliferate rapidly to restore function. If recovery does not occur within a critical timeframe, typically days to weeks, [[liver-transplantation|liver transplantation]] becomes the only life-saving option.
What is the difference between acute and chronic liver failure?
The fundamental difference lies in the speed of onset and the presence of pre-existing liver disease. [[Acute-liver-failure|Acute liver failure]] develops rapidly, within days or weeks, in individuals with previously healthy livers. It is characterized by sudden, severe liver cell death and the rapid development of complications like [[hepatic-encephalopathy|hepatic encephalopathy]] and [[coagulopathy|coagulopathy]]. In contrast, [[chronic-liver-failure|chronic liver failure]] is the end stage of long-standing liver disease, such as [[cirrhosis|cirrhosis]], which develops gradually over months or years due to conditions like [[hepatitis-c|Hepatitis C]], [[alcoholic-liver-disease|alcohol abuse]], or [[non-alcoholic-fatty-liver-disease|NAFLD]].
What immediate steps should be taken if acute liver failure is suspected?
If acute liver failure is suspected, immediate medical attention is paramount. Call emergency services (e.g., 911 in the US) or go to the nearest emergency department without delay. If [[acetaminophen-overdose|acetaminophen]] overdose is a possibility, inform medical personnel immediately, as prompt administration of [[n-acetylcysteine|N-acetylcysteine]] is critical. Avoid any further exposure to potential hepatotoxins, including alcohol and certain medications. Medical professionals will initiate diagnostic tests, provide supportive care, and determine the need for specialized interventions like [[liver-transplantation|liver transplantation]].
Are there any preventative measures for acute liver failure?
Prevention strategies focus on avoiding known causes. This includes adhering strictly to recommended dosages for [[acetaminophen|acetaminophen]] and other over-the-counter medications, and being aware of potential interactions. Vaccination against [[hepatitis-a|Hepatitis A]] and [[hepatitis-b|Hepatitis B]] is crucial. Avoiding illicit drug use and excessive alcohol consumption can prevent [[alcoholic-liver-disease|alcoholic liver disease]] and reduce the risk of [[drug-induced-liver-injury|drug-induced liver injury]]. Safe handling and identification of wild mushrooms, particularly avoiding the [[amanita-phalloides|death cap mushroom]], is vital. For individuals with known autoimmune conditions, regular medical monitoring is important.