Nonalcoholic Fatty Liver Disease | Vibepedia
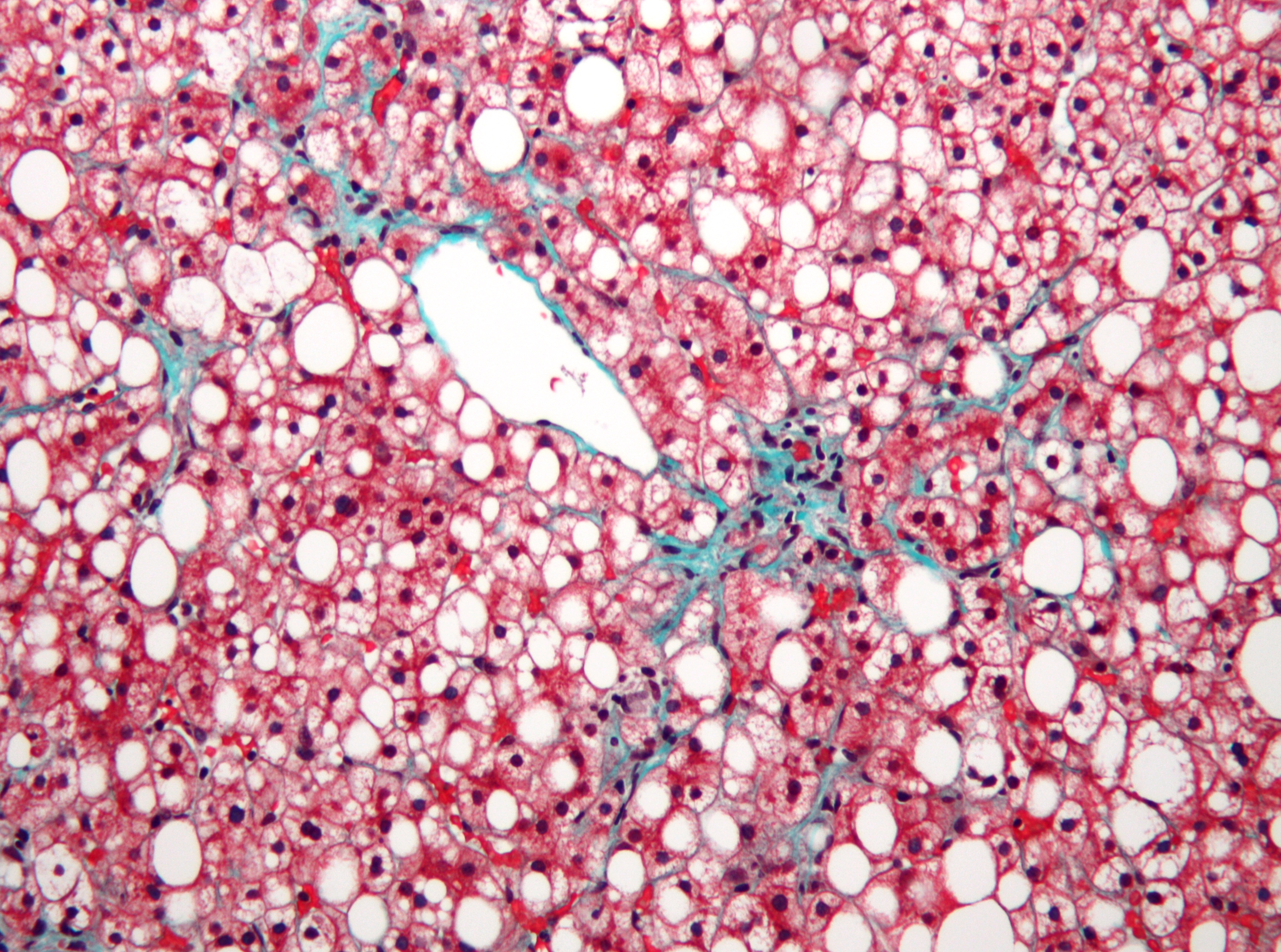
Metabolic dysfunction–associated steatotic liver disease (MASLD), formerly known as nonalcoholic fatty liver disease (NAFLD), is a pervasive medical condition…
Contents
Overview
The recognition of fatty liver disease not linked to alcohol consumption has evolved significantly. Early descriptions of 'fatty liver' date back to the early 20th century, but it wasn't until the late 1970s and early 1980s that researchers began to systematically describe a distinct entity they termed 'non-alcoholic fatty liver' (NAFL) in patients without a history of significant alcohol intake. The term 'non-alcoholic steatohepatitis' (NASH), a more inflammatory and potentially progressive form, was coined by [[neil-shapiro|Neil Shapiro]] and colleagues in 1980. For decades, this condition was often overlooked, considered benign, and primarily associated with [[obesity|obesity]]. However, as global rates of [[metabolic-syndrome|metabolic syndrome]] and [[type-2-diabetes|type 2 diabetes]] surged in the late 20th and early 21st centuries, the prevalence and clinical significance of NAFLD became undeniable, prompting a re-evaluation and ultimately a renaming in 2023 to MASLD by leading liver associations to better reflect its underlying metabolic drivers.
⚙️ How It Works
At its core, MASLD is a consequence of metabolic dysregulation, primarily insulin resistance. When the body's cells don't respond effectively to insulin, glucose and fatty acids accumulate in the bloodstream. The liver, a central metabolic organ, takes up excess fatty acids, leading to their accumulation within hepatocytes (liver cells). Initially, this fat buildup (steatosis) might be asymptomatic. However, in susceptible individuals, this fat accumulation, coupled with other metabolic insults like oxidative stress and inflammation, can trigger a more aggressive process known as MASH. MASH involves inflammation and hepatocellular injury, which can lead to the formation of scar tissue (fibrosis). Over time, this fibrosis can progress to cirrhosis, a severe and irreversible scarring of the liver, and increase the risk of [[liver-cancer|liver cancer]].
📊 Key Facts & Numbers
The scale of MASLD is staggering. Globally, it is estimated to affect approximately 25% of the adult population, translating to over 1.5 billion people. In the United States alone, over 100 million individuals are estimated to have MASLD. The prevalence is even higher in individuals with [[obesity|obesity]] (up to 90%) and [[type-2-diabetes|type 2 diabetes]] (up to 70%). The economic burden is also immense, with estimates suggesting that MASLD and its complications cost the U.S. healthcare system tens of billions of dollars annually, a figure projected to rise significantly. By 2030, it's predicted that NASH-related cirrhosis could lead to over 60,000 liver transplants and 100,000 deaths per year in the U.S. alone, highlighting its dire trajectory.
👥 Key People & Organizations
Key figures in understanding and combating MASLD include [[scott-kleiner|Scott Kleiner]], a leading researcher in NASH pathogenesis and drug development, and [[neil-theise|Neil Theise]], who has contributed significantly to understanding liver histology and disease progression. Organizations like the [[american-association-for-the-study-of-liver-diseases|American Association for the Study of Liver Diseases (AASLD)]], the [[european-association-for-the-study-of-the-liver|European Association for the Study of the Liver (EASL)]], and the [[asian-pacific-association-for-the-study-of-the-liver|Asian Pacific Association for the Study of the Liver (APASL)]] have been instrumental in defining diagnostic criteria, developing clinical guidelines, and advocating for research. Pharmaceutical companies such as [[madrigal-pharmaceuticals|Madrigal Pharmaceuticals]] (with its drug Rezdiffra) and [[gilead-sciences|Gilead Sciences]] are at the forefront of developing novel therapeutic agents targeting MASH.
🌍 Cultural Impact & Influence
MASLD's rise mirrors the broader cultural shift towards more sedentary lifestyles and processed food consumption, making it a potent symbol of modern metabolic ill-health. Its 'silent' nature means it often goes undetected until advanced stages, contributing to a sense of unease and a growing awareness of the hidden health crises within seemingly healthy populations. The rebranding to MASLD itself reflects a cultural shift in understanding, moving away from a simplistic 'fatty liver' label to one that emphasizes the complex interplay of metabolic factors. This condition is increasingly discussed in mainstream media, not just as a medical issue but as a consequence of societal trends, influencing public health campaigns and dietary recommendations.
⚡ Current State & Latest Developments
The landscape of MASLD is rapidly evolving, particularly with the recent renaming to MASLD and MASH in June 2023, a move aimed at destigmatizing the condition and better reflecting its metabolic origins. This shift was driven by a consensus among major liver associations, including the AASLD, EASL, and APASL. Crucially, 2024 has seen the first FDA approval of a drug specifically for MASH: [[madrigal-pharmaceuticals-rezdiffra|Madrigal Pharmaceuticals' Rezdiffra (resmetirom)]], marking a significant milestone in treatment options. Ongoing clinical trials are exploring numerous other therapeutic targets, including agents for [[fibrosis|fibrosis]] reversal and inflammation reduction, signaling a new era of pharmacological intervention beyond lifestyle changes. Research is also intensifying on non-invasive diagnostic tools, such as advanced imaging techniques and biomarker panels, to improve early detection.
🤔 Controversies & Debates
A central debate revolves around the optimal diagnostic approach. While liver biopsy remains the gold standard for staging MASH and fibrosis, its invasive nature and associated risks have spurred the development and validation of non-invasive methods. These include blood tests (e.g., [[fibrosis-4-index|Fibrosis-4 Index (FIB-4)]], [[enhanced-liver-fibrosis-test|Enhanced Liver Fibrosis (ELF) test]]) and imaging techniques like [[transient-elastography|transient elastography]] (e.g., [[fibroscan|FibroScan]]). Another point of contention is the best strategy for managing MASLD, with ongoing discussions about the relative importance of diet, exercise, and pharmacotherapy, especially in diverse patient populations with varying comorbidities. The recent renaming itself has sparked debate, with some arguing it doesn't go far enough to address the societal drivers of the disease.
🔮 Future Outlook & Predictions
The future of MASLD management is poised for significant transformation. Beyond the newly approved Rezdiffra, numerous drug candidates are in late-stage clinical trials, targeting various pathways involved in fat accumulation, inflammation, and fibrosis. Experts predict a future where MASLD is managed with a combination of lifestyle interventions and personalized pharmacotherapy, potentially including drugs that can reverse liver fibrosis. Furthermore, advancements in [[genetics|genetics]] and [[epigenetics|epigenetics]] may lead to better risk stratification and the identification of individuals most likely to progress to severe liver disease. The focus is shifting from merely slowing progression to actively healing the liver, a prospect that was unthinkable just a decade ago.
💡 Practical Applications
The primary practical application of understanding MASLD lies in its prevention and management through lifestyle modifications. This includes adopting a balanced diet, rich in fruits, vegetables, and whole grains, while limiting intake of [[processed-foods|processed foods]], sugary drinks, and saturated fats. Regular physical activity, aiming for at least 150 minutes of moderate-intensity exercise per week, is crucial for improving insulin sensitivity and promoting weight loss. For individuals diagnosed with MASLD, regular medical monitoring is essential to track disease progression and manage associated conditions like [[hypertension|hypertension]] and [[dyslipidemia|dyslipidemia]]. The development of new pharmacological treatments offers further avenues for intervention, particularly for those with MASH and significant fibrosis.
Key Facts
- Category
- science
- Type
- topic